Page 533 - Motor Disorders Third Edition
P. 533
DIABETIC NEUROPATHY / 515
(A) (B)
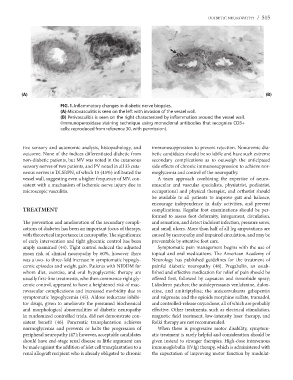
FIG.?1.?Inflammatory changes in diabetic nerve biopsies.
(A) Microvasculitis is seen on the left with invasion of the vessel wall.
(B) Perivasculitis is seen on the right characterized by inflammation around the vessel wall.
(Immunoperoxidase staining technique using monoclonal antibodies that recognize CD3+
cells; reproduced from reference 30, with permission).
tive sensory and autonomic analysis, histopathology, and immunosuppression to prevent rejection. Nonuremic dia-
outcome. None of the indices differentiated diabetic from betic candidates should be so labile and have such extreme
non-diabetic patients, but MV was noted in the cutaneous secondary complications as to outweigh the anticipated
sensory nerves of two patients, and PV noted in all 33 cuta- side effects of chronic immunosuppression to achieve nor-
neous nerves in DLSRPN, of which 15 (45%) infiltrated the moglycemia and control of the neuropathy.
vessel wall, suggesting even a higher frequency of MV, con-
sistent with a mechanism of ischemic nerve injury due to A team approach combining the expertise of neuro-
microscopic vasculitis. muscular and vascular specialists, physiatrist, podiatrist,
occupational and physical therapist, and orthotist should
TREATMENT be available to all patients to improve gait and balance,
encourage independence in daily activities, and prevent
The prevention and amelioration of the secondary compli- complications. Regular foot examinations should be per-
cations of diabetes has been an important focus of therapy, formed to assess foot deformity, integument, circulation,
with theoretical importance in neuropathy. The significance and sensation, and detect indolent infection, pressure sores,
of early intervention and tight glycemic control has been and small ulcers. More than half of all leg amputations are
amply examined (44). Tight control reduced the adjusted caused by neuropathy and impaired circulation, and may be
mean risk of clinical neuropathy by 60%, however there preventable by attentive foot care.
was a two- to three-fold increase in symptomatic hypogly-
cemic episodes and weight gain. Patients with NIDDM for Symptomatic pain management begins with the use of
whom diet, exercise, and oral hypoglycemic therapy are topical and oral medications. The American Academy of
usually first-line treatments, who then commence right gly- Neurology has published guidelines for the treatment of
cemic control, appeared to have a heightened risk of mac- painful diabetic neuropathy (48). Pregabalin, an estab-
rovascular complications and increased morbidity due to lished and effective medication for relief of pain should be
symptomatic hypoglycemia (45). Aldose reductase inhibi- offered first, followed by capsaicin and isosorbide spray;
tor drugs, given to ameliorate the presumed biochemical Lidoderm patches; the antidepressants venlafaxine, dulox-
and morphological abnormalities of diabetic neuropathy etine, and amitriptyline; the anticonvulsants gabapentin
in randomized controlled trials, did not demonstrate con- and valproate; and the opioids morphine sulfate, tramadol,
sistent benefit (46). Pancreatic transplantation achieves and controlled-release oxycodone, all of which are probably
normoglycemia and prevents or halts the progression of effective. Other treatments, such as electrical stimulation,
peripheral neuropathy (47); however, acceptable candidates magnetic field treatment, low-intensity laser therapy, and
should have end-stage renal disease as little argument can Reiki therapy are not recommended.
be made against the addition of islet cell transplantation to a
renal allograft recipient who is already obligated to chronic When there is progressive motor disability, symptom-
atic treatment is rarely helpful and consideration should be
given instead to stronger therapies. High-dose intravenous
immunoglobulin (IVIg) therapy, which is administered with
the expectation of improving motor function by modulat-